Well-Placed: The impact of Big Local on the health of communities

How can communities prevent illness and create their own good health? Could investment at the grassroots help ease the burden on the NHS?
To find out, we analysed the impact of Local Trust’s Big Local project. How did this scheme, which gave places £1 million to spend improving their areas, impact health and wellbeing? And what lessons does it have for the wider healthcare system?
Author Imran Hashmi introduces the report
Executive Summary
Introduction
Our health system is under extreme stress. Demand for health and care services is rising faster than their ability to respond. Years of underfunding and the impact of the COVID-19 pandemic are presenting immediate challenges manifesting in rising waiting lists and intolerable workforce pressures. But underlying this, systemic pressures due to our ageing population with ongoing, more complex care needs, and rising inequality are playing a big role.
Our traditional model of healthcare provision is hospital-based, clinically led and focused on managing treatment. There is widespread recognition that we need to shift the centre of gravity within our system of health and care towards prevention, and away from expensive acute reaction which is costly for public finances and worse for people’s experience and outcomes.
This would mean addressing the social determinants of health outcomes – the range of physical, social and environmental factors which many experts agree are more important for good health than services alone. Health inequalities present a further systemic challenge. These inequalities are significant, evident through the gap in life expectancy where women and men living in the most deprived areas of the country can expect to live eight and 9.4 years less respectively than people in the least deprived areas. While health inequalities are linked clearly to deprivation, there are also important connections between health inequalities and place which add further complexity to the policy response needed.
In this context, the role of communities is increasingly important. Although they exist outside the boundaries of formal healthcare institutions, there is evidence of improved health outcomes from a range of community-led initiatives. From the perspective of our highly pressurised healthcare system, they exist on the margins and are a neglected asset when it comes to formal planning, commissioning and resource allocation. But there are reasons to be optimistic that the formal system of healthcare provision is shifting in a direction that in principle is more able to recognise the value of community-led approaches. Integrated Care Systems (ICSs) were formalised in 2022 as partnerships bringing together NHS organisations, local authorities and other relevant bodies to take collective responsibility for planning services, improving health and reducing inequalities across places.
The ICSs cover large geographical areas, typically around one million people, but within each ICS footprint two smaller scales are formally recognised – ‘place’ partnerships and ‘neighbourhoods’. ICSs are underpinned by the principles of subsidiarity – which means they should consider whether decisions need to be taken at a system-wide level or if they can be taken more locally. As a result, some Integrated Care Boards (ICBs) have pioneered different ways of working with people and communities who face health barriers and unequal outcomes. However, in the context of extreme pressure on services and the workforce, there has not yet been a notable shift towards a different way of working within systems to further enable and value community-led approaches to health and wellbeing.
This research set out to understand more about the role of one particular community-led approach to health and wellbeing. The Big Local programme is focused on 150 ‘hyperlocal’ neighbourhoods, which shared common characteristics of high levels of deprivation, low levels of social capital and lower-than-average health outcomes. Each were given £1 million to spend over the course of 10-15 years from 2010-12 onwards. By placing considerable resource and autonomy over decision-making in the hands of communities, the model offers a unique insight into how communities would understand, identify and pursue their own priorities.
For the wider health system, the Big Local model provides a unique source of evidence for the efficacy of community-led initiatives on improving health and wellbeing outcomes. The experience of Big Local areas is instructive for how emerging local health systems organised around places recognise, work with and support community-led initiatives for improved health and wellbeing. These initiatives could have significant impacts not just for individual experience and outcomes, but hold the potential to alleviate demand pressures on formal healthcare provision.
Key Findings
Our research identified a wide range of health-related activity being supported by Big Local partnerships, revealed through a review of literature and a series of interviews with those directly involved. The diagram below summarises these key findings. We identify four core conditions that enabled Big Local partnerships to set up, fund and run health activities. We identified seven different themes for this activity, which address different aspects of health and wellbeing in those communities. The impact generated by this activity is observed through the framing of three key social determinants of health outcomes.
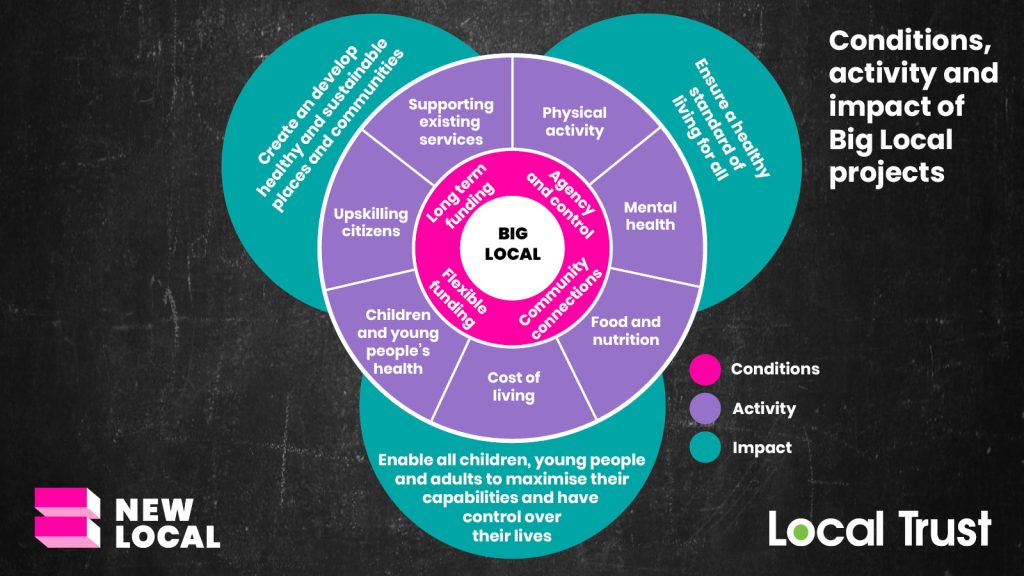
Core conditions for community-led initiatives that support health and wellbeing
At the heart of the Big Local model are four core conditions that help enable community-led action on health and wellbeing. While each one of these conditions is important in its own right, together they provide the environment for communities to identify and lead initiatives that respond to and support residents’ health and wellbeing. The four identified conditions are:
- Agency and control: Placing power and control in the hands of communities through resident-led decision making.
- Community connections: Big Local partnerships are embedded within their communities and understand the unique challenges they face. They have therefore been able to more effectively design interventions that address local issues and reach the most in need groups of people.
- Flexible funding: Flexibility of funding has proved responsive to communities’ identified priorities and circumstances, ensuring support meets needs rather than being restricted to a pre-determined theme, type of intervention or condition.
- Long-term funding: A long-term funding approach has built community capacity and capability while designing effective interventions for the long term.
Seven areas of activity to support health and wellbeing
The four conditions enabled Big Local partnerships to work with their communities to design and fund activities as they felt necessary. This is an important feature of the Big Local model – ensuring local communities can identify shared priorities and collectively agree what would support them meaningfully.
Our research found a wide range of activities that we grouped into seven themes. Some meet general ongoing needs such as support for physical activity and good nutrition, and some are clearly shaped by circumstances as they have manifested over the last decade; responding to deteriorating mental wellbeing after the pandemic and the pressures of the cost-of-living crisis. These seven themes and the specific activity within each are presented on the table below:
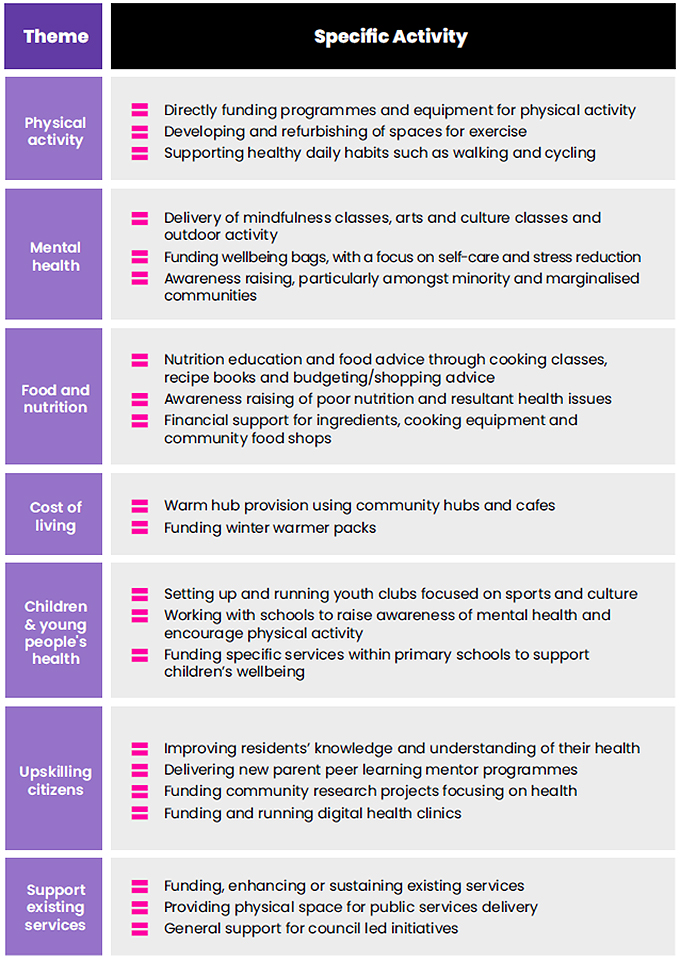
The impact of community-led initiatives on health and wellbeing
Our research identified important impacts on health and wellbeing. In general, quantitative findings from the census indicate that over the decade of the programme’s operation, the health of residents in Big Local areas was stronger over this period than the rest of the population.
There were statistically significant improvements in residents reporting greater than average increases in ‘very good’ health compared to non-Big Local areas between 2011 and 2021. Other studies are also starting to show health impact, primarily through improvements in residents’ wellbeing.
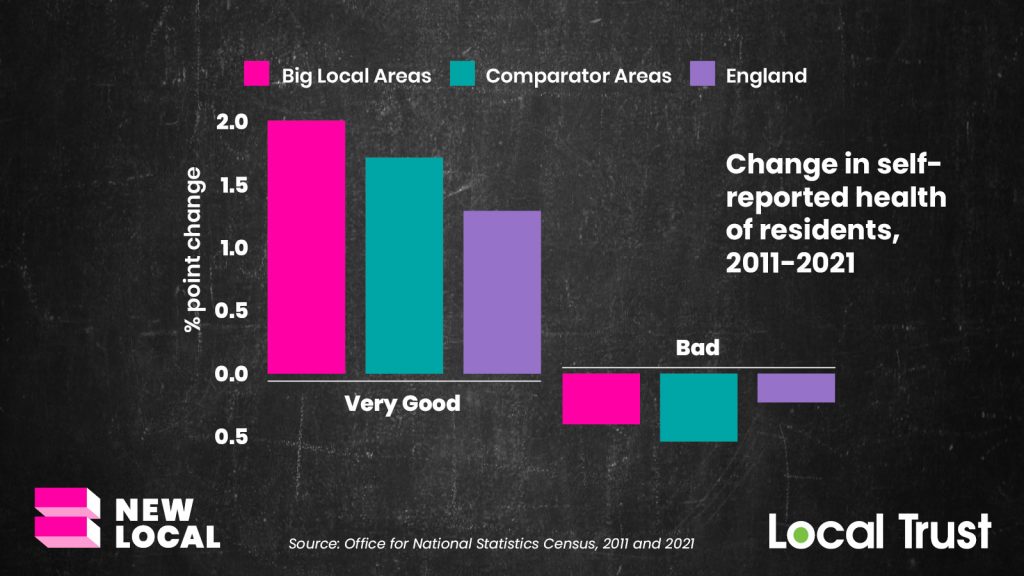
Our research used the framing of three key social determinants of good health to explore the impact of the Big Local partnerships as observed and reported by members through our interviews. With the right conditions to address community defined priorities, Big Local partnerships designed activities that focused not on formal health outcomes but on a broader range of issues that improve health:
- Enabling a healthier standard of living for all.
- Enabling children and young people to maximise their capabilitiesand have control over their lives.
- Creating and developing healthy and sustainable places for all.
Limiting factors facing community-led initiatives on health and wellbeing
The activity and impact realised by Big Local partnerships on health and wellbeing has progressed despite facing a series of obstacles which limit the scale and impact of the activities. Our research found three main obstacles which limit the degree of impact from Big Local partnerships and their ability to reduce demand for formal health provision.
Recommendations
For the healthcare system
The report makes three recommendations for ICSs, and the wider formal healthcare system, if the impact of community-led initiatives on health outcomes and demand pressures is to be fully realised in the future.
- Recommendation 1: Health system partners at all levels should develop a deeper shared understanding of where and how hyperlocal deprivation manifests within their geographies.
- Recommendation 2: Health systems should aim to deepen and expand community-led approaches to health and wellbeing, adopting a ‘test and learn’ approach to measure their impact on outcomes and demand.
- Recommendation 3: System partners should commit to shifting resource towards investment in community-led health and wellbeing initiatives, as part of a wider rebalancing of spend towards prevention.
For Big Local partnerships
This report makes two recommendations for Big Local partnerships to improve their chances of working effectively with the formal healthcare system, despite identified limiting factors:
- Recommendation 1: Consciously and methodically build local links and relationships with the full range of stakeholders that work in health and wellbeing.
- Recommendation 2: Demystify and clearly evidence the work and impact of Big Local groups.
Conclusion
Big Local partnerships have created the conditions for successful community-led health initiatives. Their unique position in understanding the community, placing power and control in the hands of the community, and providing long term and flexible funding enabled a wide range of community-led health activity that has had direct and indirect benefits for health outcomes. This activity and corresponding impact have been delivered despite facing significant institutional barriers.
Given the challenges facing the formal health system, policy makers need to urgently recognise the sustainability, value and contribution that Big Local and hyperlocal initiatives can make on improving the health of the population.
 Join our mailing list
Join our mailing list






